The Future is Allied: How Allied Health Programs are Preparing Students for In-Demand Jobs
Adaptations is a series of interviews with educators from around the world, representing diverse backgrounds, disciplines and institutions. These interviews examine how educators are adapting to the ever-changing education landscape and how the built environment helps or hinders them in that effort.
This interview has been edited for length and clarity.
Late last year, we posted Part 1 of our second installment of Adaptations, highlighting our interview with Dr. Phillip Nicotera and Dean Jeff Gricar of Houston Community College, who provided insight into the major changes and shifts taking place in community colleges across the United States.
In Part 2 of this installment, Dr. Nicotera and Dean Gricar speak with HDR about how the allied health programs at HCC's Coleman College for Health Sciences are evolving to meet the demands of a changing healthcare system.
According to the U.S. Bureau of Labor Statistics, employment in healthcare occupations is projected to grow an average of 18 percent between 2016 and 2026, a rate much faster than the 7 percent job growth expected for all occupations combined. Some jobs, within the healthcare category, are expected to grow at rates approaching 30 percent including occupational therapy assistants (28 percent), physical therapy assistants (30 percent), and medical assistants (29 percent). Increased demand in healthcare occupations is largely attributed to an aging population, creating more demand for healthcare services. Community colleges provide a significant portion of the nation’s allied health job training.
Responding to Rapidly Evolving Technology
HDR: What have been the primary changes in how health sciences are taught over the last ten years?
Gricar: I think the major changes in health sciences are related to technology, which can be very hard to keep up with. As soon as you learn one new technology, something else emerges, so you're constantly trying to catch up. Many people assume younger students are really good with the technology. But the reality is they're good with their phone; it's not necessarily everything else.
HDR: So how do you keep up with these changes in technology?
Nicotera: All of our programs have advisory committees — individuals that are currently working in the profession — that meet quarterly. We discuss the changes that they are seeing and they advise us on things that we may need to change in our curriculum.
Additionally, our faculty are also clinical instructors, which means that they are out in the clinical communities with our students. Also, some of them are required to work a limited number of hours to maintain their licensure. So they bring feedback from their experiences back to us, so we can make adjustments to the curriculum, as needed.
Leveraging the Game-Changing Power of Simulation
HDR: What other changes have impacted health sciences education?
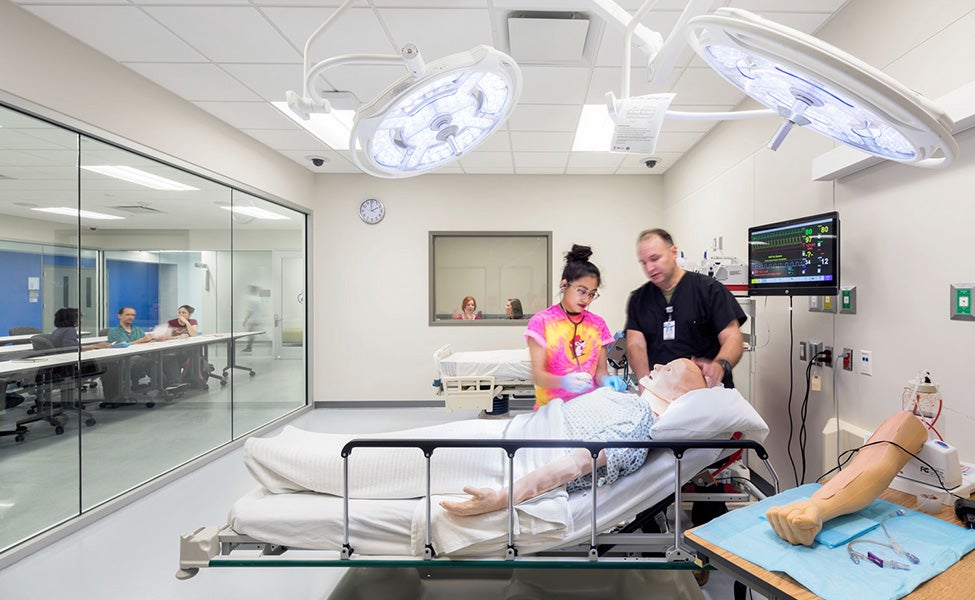
Nicotera: The increase in the use of simulation has been dramatic. Ten years ago, it was in its infancy, and we've seen it grow tremendously for several reasons:
- Number one is the level of competition for clinical sites. Many of our clinical sites have key priorities around patient safety and patient outcomes. So they have to limit the number of students that are in any clinical site at one time to be able to maintain that balance. With clinical sites somewhat limited, simulation has been able to take their place in many respects.
- Secondly, simulation allows us to provide hands-on experiences to students that they may never get in a real clinical situation. You could be at a clinical site, and you may never see a person have a heart attack. While medically, it’s great that didn’t happen, from an education standpoint it is still helpful to be able to simulate that, so if a student runs into it once they are out in the field, they know what to do.
- Finally, all of our programs are accredited by specialized or programmatic entities that provide standards. These accrediting bodies are starting to really understand the value of simulation and have allowed us to increase the amount of simulation we are able to allocate as clinical time.
HDR: Is there a requirement for a certain amount of time in simulation before students go into the clinical setting with real patients?
Nicotera: Simulation is woven into the curriculum and the program, and that's the way it should be done, so we don't always do simulation before a student goes out into a clinical setting. Many programs, such as nursing, send students out before they've had any simulation, but they have had skills training (in a skills lab) before they go. We have a lot of skills labs, so they're practicing skills in other ways, not only in the simulation.
HDR: Are there faculty who have had difficulty adapting to the expanded use of simulation?
Gricar: I think the main challenge is not necessarily seeing the value that the simulation holds, because I think instructors see how powerful it can be. If they simulate a patient dying, you'd be surprised at the number of students that will just break down because of how real it seems. So it's not necessarily that they don't understand the power, it’s just that it’s new. It's something we haven't done before, and that is the hindrance in getting everybody on board to use it more often.
Nicotera: We have repurposed one of our faculty positions to be a simulation instructor for nursing. Part of her role is to help demystify the technology with her colleagues, help demonstrate the value, and make them more comfortable with using simulation.
Positioning Students for Interdisciplinary Care
HDR: How do you see your role, as an institution, in the movement towards comprehensive care and enabling collaboration across disciplines?
Gricar: One of my main goals, with the dean of nursing, is to get everybody working together. To get us out of our silos, so that students understand how important each of the other roles on the health care team actually are. I think that will be a key goal in the simulation center — trying to get everybody involved and making it just like a real hospital setting, where a team of professionals work together.
Linking Space to New Educational Opportunities
HDR: How important do you see your location within the Texas Medical Center to your curriculum, your mission?
Nicotera: The new Coleman Health Science Tower, with the bridge connecting directly to the campus, now changes the footprint of who we are. It attracts students who are asking: Where do I want to go to school? Do I want to go out to some office building in the middle of nowhere, or do I want to get my healthcare training at the Texas Medical Center? Around 55 to 60 percent of our graduates end up working at TMC.
While our location is a very important selling point for students, it also helps us attract adjunct faculty because they can come here and teach right after work.
Gricar: I think the space (in the new building) is going to improve the quality of instruction, too. The students are going to have the space to be able to do what they need to do and not feel cramped.
Nicotera: Part of what we hope to do in the next few years is to become more involved in the Texas Medical Center. We've got some nice space here and some extra space, for now. We are interested in working with TMC on ways to use the space in this building to benefit the wider campus. We think the new building could help us become a more active part of TMC.
For more information about Houston Community College Coleman Health Science Tower:
The Job Readiness Factor: Community Colleges in the Face of Changing Industries
Houston Community College Coleman Health Science Tower