Designing for Health Sciences Education: Planning Considerations for Clinical Skills and Simulation Centers
This is the fourth article in six-part Designing for Health Sciences Education series.
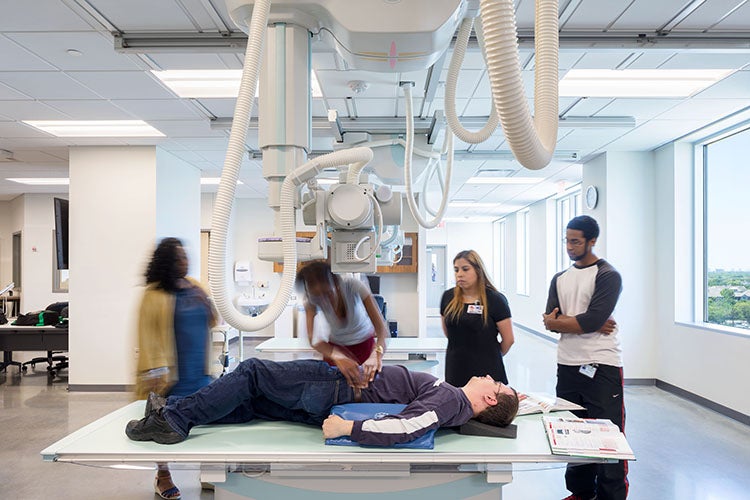
Providing opportunities for students to practice the concepts they have learned through hands-on exercises that mimic the clinical environment is an essential aspect of health sciences education environments for all professions. These opportunities most commonly occur in the simulation and clinical skills centers. All of these functions can overlap and/or share space, and all of them provide virtual and physical spaces for skills to be taught and mastered.
In the simplest terms, the simulation center provides the opportunity for all denizens of a health sciences center, from the newest nursing student to the most advanced surgeon, to practice a procedure before actually performing it on a live patient. This article, the fourth in our series on Designing for Health Sciences Education, explores the operational and design considerations for simulation centers.
Determining the Operational Goals of a Simulation Center
The ideal location of a simulation center within a medical center complex depends on its projected constituents and range of activities. If its primary purpose is to train students — medical, nursing, and allied health students — then designing it so that it can serve for Objective Structured Clinical Exams provides ideal flexibility. If designed appropriately, these simulation centers can be very flexible for three much needed uses: general simulation activities either with standardized patients or with low or high-fidelity manekins, formal OSCE exams, and group study.
While these more general simulation centers can sometimes be dedicated to use by medical students only, or nursing students only, this is rarely the best stewardship of a valuable resource. Since these students have quite stringent schedules, including class time, group and individual study, clinical rotations, working as patient advocates, and simply living their lives, dedicating a simulation center to a single group often means that it will sit empty much of the time.
On the flip side, once a simulation center is up and running for one department or discipline, the idea quickly catches on, and other disciplines see what is happening, think of ways to adapt the idea to their own practice, and sign up for time in the center. These simulation centers end up needing to handle more activity than anticipated and run into multiple issues with scheduling, lack of sufficient storage, assembly and debrief space, and insufficient staff to run the simulations. This underscores why comprehensive campus planning with all key stakeholders is so important when planning a comprehensive simulation center.
Specialized Simulation Centers
If the primary purpose of the simulation center is to support highly specialized activities and procedures for already practicing nurses, surgeons or other professionals, a smaller, more focused simulation center located close to a specialty group might make sense. For example, a surgeon may want to practice a specific procedure on a specific type of patient or condition just before entering the OR to perform it for real. An orthopedist may want to work with a standardized patient who is portraying a specific gait issue before undertaking that work with the real patient.
Establishing the Right Program
If the simulation center is to be used for OSCEs, the planning must take into consideration the number of students in the cohort and the number of exam rooms that will ideally allow those students to rotate through the suite in a logical way. Consider a typical scenario:
- There is a class of 144 students using the simulation center to take their OSCEs
- Each student takes anywhere from 5-20 minutes in each room in the suite, where they encounter a different standardized patient.
- A suite of 12 rooms will allow 12 students at a time in the OSCE. So a single rotation of students may take anywhere from an hour to an afternoon.
- As a result, it may take up to a week for that entire class to take a single OSCE.
- There could be several OSCEs for a single class during their third and fourth years, so the amount of time needed for these spaces is substantial, particularly if the suite is shared with other disciplines.
In addition to rooms that mimic outpatient clinic exam rooms, a simulation center must include specialty rooms for simulations as well. These may include exam rooms that are larger for interprofessional education activities and mock hospital rooms that include headwalls and toilet facilities and are designed exactly as the teaching hospital’s patient rooms are designed. The same rooms may be used for nursing, medical, pharmacy and other students who will be simulating the activities specific to their discipline.
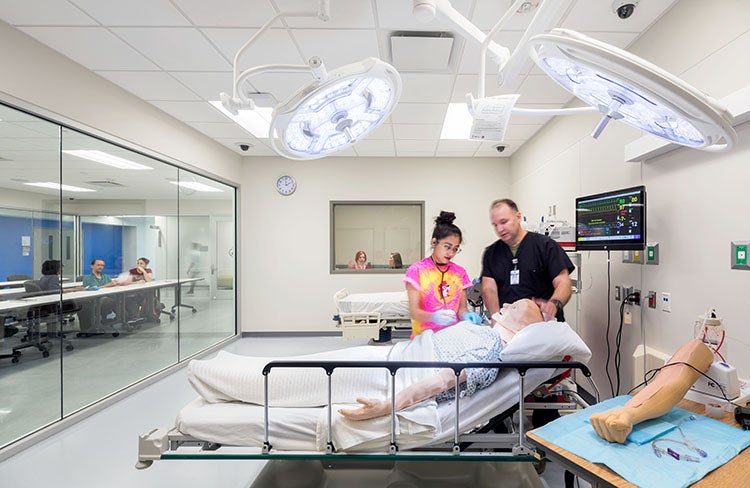
Even more specialized rooms such as an OR, trauma bay, OB-GYN, intensive care unit, neonatal intensive care unit, and infusion rooms may also form part of the simulation center’s program. If first responders are using the center, simulated ambulance bays and other emergency activity environments may be part of the program. A home living room or apartment may accommodate nursing students as well as first responders. In design, care must be taken that the room looks and feels like the real clinical experience, but also has the space for active participants, observers and trainers to move around. With the right design, these rooms can also be used for hospital staff to be taught proper cleaning procedures, porters can simulate how to move patients appropriately, and appropriate protocols for different conditions can be practiced in these spaces.
In addition to simulation rooms that support standardized patients or mannikins, there are several clinical skills that are related to medical specialties. Scrubbing for surgery, knot-tying, phlebotomy and mastery of minimally invasive surgical techniques are other common skills that must be mastered. Often a common lower-tech clinical skills lab, that is always open for both teaching and practice, is designed for this purpose.
Key Design Factors in Simulation Centers
A simulation center has a complex set of operations that its design can either aid or hamper. Key design factors to consider include:
- Entry Sequence: The entry sequence should provide a briefing room large enough for the biggest group to be seated and hear the introduction to the encounters that will occur. This may or may not be within the simulation suite, but it should be close enough that students can enter quickly once they have been through the introduction.
- Pathways for Standardized Patients: Standardized patients should have clear pathways to enter the suite and access their changing and break areas. The corridor system should allow them clear access from changing and break areas into the exam rooms without crossing paths with the students and without going through any public areas (since they often are gowned). These standardized patient facilities must be large enough to accommodate the number of standardized patients that are likely to be there at one time.
- Sufficient Exam Room Space: The number of identical exam rooms required to accommodate a full cohort in a logical fashion is typically between 12 and 20, but is dependent on class sizes.
- Debriefing Room Capacity: Typically, at least three debriefing rooms should be available for a suite of 12 exam rooms. The entry “briefing” or introductory room can also operate as a debriefing room as scheduling and traffic flow allows.
- Control Capacity: Control rooms may be decentralized or central, but there must be control capability for an instructor to direct what goes on in each room. Often one control room is located between two exam rooms, but they may be remote as well.
Equipment, Storage, and Staffing Considerations
Equipment: When planning a simulation center, the types and resulting costs of equipment and technology to be provided should not be underestimated. Some higher end mannikins are very expensive, and a center needs several different types for different tasks. The center also needs task trainers, gurneys, medical and IV supplies, etc.
Storage: Storage needs are significant, since many different types of equipment are used for short periods, then replaced by other equipment. Without sufficient storage, idle equipment invariably ends up in the corridor, interfering with traffic flow and leaving valuable equipment at risk. A minimum of ten percent of the active simulation space should be dedicated to storage, and that percentage should be greater if the suite is small and used by a wider variety of disciplines.
Staffing: Staffing requires specialists in IT who understand the technology of the mannikins as well as a director and/or manager, scheduler, and instructors. Without appropriate staff to schedule the center’s activities, to set up and take down the simulations and to operate and repair the mannikins, the suite will not be used efficiently. The most efficiently run simulation centers are usually those that serve both students and clinical functions, that are large enough and flexible enough to run different types of activities at the same time, and that are staffed with the right number of specialists to run things.
AV and IT in the Simulation Center
Audio-visual and information technology are critical to the success of a simulation center. As students encounter the “patients,” their manner, command of appropriate diagnostic and treatment techniques, and communication skills with that patient need to be clearly visible to the instructor by means of cameras or, with older technology, a one-way mirror. The encounter must be recorded, again with both caregiver and patient clearly visible, and that recording able to be played back to a group in a debriefing room, ideally immediately after it happens. Since this technology changes rapidly, providing flexible infrastructure and waiting as late as possible to specify the actual AV/IT equipment is generally the best course.
With the use of sophisticated and advanced electronics, dedicated workshop space is a must for technicians to repair manekins and evaluate electronics. Instructors need to be able to work with the center director to plan activities, and sim center staff need space to prepare course materials, etc. These support spaces are vital to the efficient and successful operation of a clinical skills and simulation center.
Conclusion
In our Adaptations conversation with Dr. Phillip Nicotera of Houston Community College a few years back, he emphasized the game-changer that simulation has been to health sciences education and the tremendous growth the use of simulation has seen over the last decade. He attributed this to the level of competition for clinical sites, the opportunities simulation centers afford students for hands-on learning experiences they might not otherwise have, and the fact that some accrediting bodies are starting to increase the number of hours in simulation that can count towards clinical time. However, renovating or planning a new simulation center can be a big undertaking.
In addition to the many considerations outlined in this article, it’s important to see the center in its greater context within the academic medical center. What operations or equipment can be shared with other labs? What are appropriate adjacencies to other learning environments and to the clinical care and research facilities on the campus to provide convenient travel for both faculty and students? Planning the center for success means anticipating that its use will increase as the demand for interprofessional education and integrated care teams increases. Sorting through these questions with professionals who understand the complexities of simulation center design is critical to the success of the center and ultimately to the health sciences program.